Key milestones
“There are great opportunities to take from this experience”
Maurice Geary, director of Orbis’ Flying Eye Hospital, on the acceleration of blended learning during COVID-19 and how the charity’s training adapted to international lockdown

Maurice Geary
16 November 2020
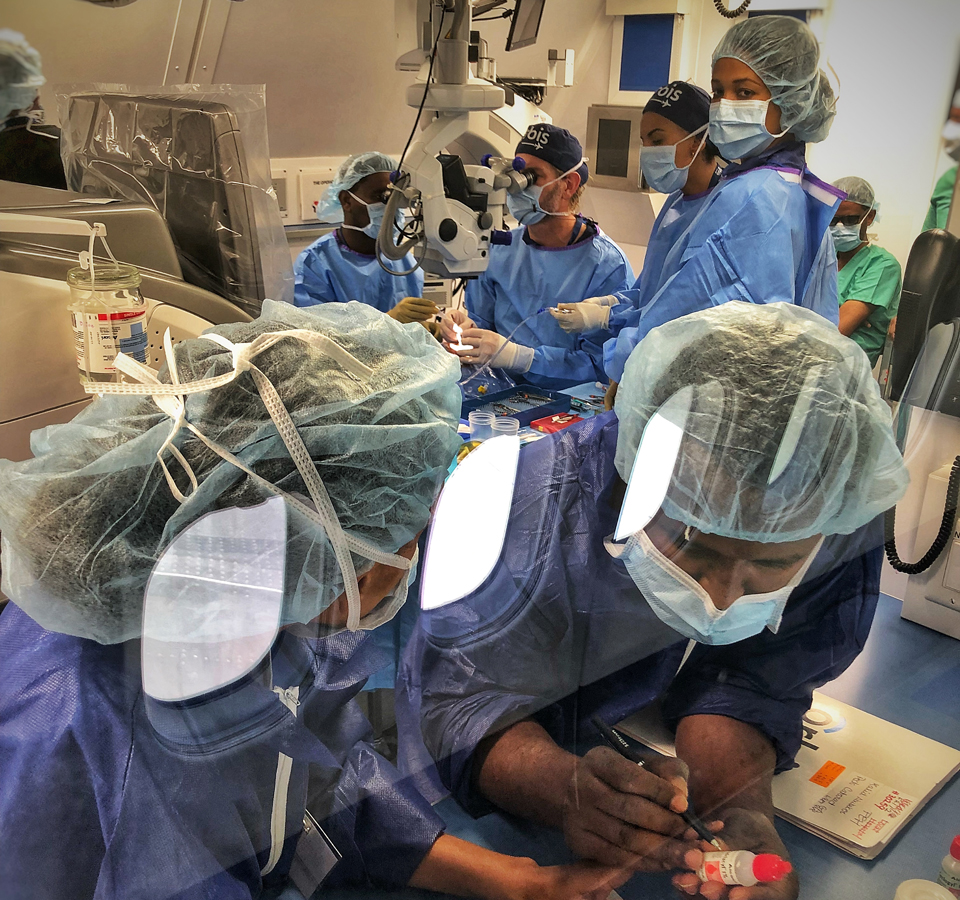
1. The Flying Eye Hospital is a training hospital, which is built inside an empty aircraft.
It was first created around 40 years ago, and the idea was to bring high quality medical training to the clinical teams, either to people or locations that couldn't normally access that level of training.That mission and that model hasn't really changed for over 40 years. What has evolved is the way that we can deliver that training. We still do live surgical training onboard the plane; we do lectures to groups. Also, in recent years, we started introducing simulation training. We use artificial eyes and high-fidelity mannequins to deliver a lot of training in a safe, simulated environment.
At Orbis, we have our own telemedicine platform, CyberSight which we use to deliver remote training. Doctors can register and do consultations. Through that they get connected with experts from around the world to discuss individual cases and surgical techniques.
2. Typically, it takes us about a year to plan and then deliver the project.
We always work through Orbis country offices and partner hospitals around the world. A year before, we will send a team, who will do an assessment of the facility and work with the management of those hospitals to identify what the training needs are and start to develop a training plan for that particular partner and that particular project.Something that I really like about the Flying Eye Hospital is that every time we deliver a project, it is tailored specifically to needs. We're not trying to do a cookie-cutter, same approach for everybody, because the needs vary so much from place to place.
We identified very quickly that our mission as a project is to deliver high-quality training to health teams around the world. That mission hasn't changed
When we do get in country, we use a combination of those different training modalities that I was talking about.
So, we might do a week of simulation training first, where we're teaching residents with artificial eyes. We'll then do a week of live surgical training, where we're teaching, doing hands-on surgical training for more experienced ophthalmologists, and also doing lectures in between the surgeries.On the plane we have a passenger seating area at the front, which we turn into our classroom during the project so we can watch the surgeries live through recording equipment in the microscope. The surgeon is also miked up, so we have live, two-way conversations during the surgery. In between the surgeries, the surgeons will come in and deliver lectures and discuss the case they just did with a group of doctors.
3. In March this year we were with the Flying Eye Hospital in Fort Worth, Texas, where, in partnership with Alcon, we were delivering a simulation training project for doctors and nurses from Bolivia.
During the middle of that project we made the very difficult decision that we were going to have to cut short the project and send everybody home for their safety. So, I made a very difficult decision. But our priority was the safety of our participants, our partners, and our staff.Once we'd made that decision, getting everybody home took about a week - my team of 28 people live in 15 different countries right across the globe, so it was no small feat to get everybody home with such short notice.
Once we got everybody home, we sat down as a team and really thought about what we were going to deliver this year, since the in-person training that we would typically do was not going to be possible for at least the short-term. We identified very quickly that our mission as a project is to deliver high-quality training to health teams around the world. That mission hasn't changed. That's still our mission for the year.

We were quite lucky at Orbis, in that we did have infrastructure in place. We have the CyberSight telemedicine platform. We have expertise within the organisation in delivering remote training. We decided that we wanted to deliver training to the clinical teams in the five locations that we were scheduled to visit in 2020: Bolivia, Zambia, Cameroon, Mongolia and India. We had already started working with partner institutions in those countries to deliver in-person training in 2020. So, we decided, okay, let's deliver remote training to those same clinical teams.
Once we had that decision made, we were able to work with our colleagues and say, ‘this is our plan for the year. How are we going to do it?’ Because we had that in-house expertise, once the decisions were made it was quite quick for us to change to delivering remote training.
4. We were able to bring in advisers to give us guidance on how to deliver remote training.
We had also invested in some training for the Flying Eye Hospital team in delivering remote training. Something we were already working towards was a sort of a blended learning approach, where we were going to combine that remote learning through CyberSight with in-person training. So, we had those foundations in place.One of the challenges that we faced at the start was really identifying what the demand was going to be like from our partners. This was back in April, when things were changing very quickly. There was a huge amount of uncertainty globally: what was going to happen with the pandemic? So, a challenge was working with partners to establish: is there going to be demand for this type of training? Will people have connectivity? Practical, logistical challenges.
5. It was a combination of challenges and things that turned into opportunities.
We were worried about connectivity in some places, and also people's available time for the training. A lot of these clinical teams were being pulled into COVID-19 response. We were able to work with teams on the best ways to address that.A lot of the training is a combination of online, self-paced learning, which is then followed up with live sessions. Orbis has a huge volunteer faculty - international experts who volunteer their time to deliver training when we do the traditional Flying Eye Hospital projects. We were able to pull those experts in to deliver live sessions through Zoom, so that people could access that remotely in their own homes.
With those live sessions, we really tried to make it interactive. So, it'd be some short lectures, but a lot of interactive Q&As, so that we could really engage those participants around the world. We also record all the sessions and edit them afterwards so that people that can't join the live session at the time can go back and still view them later.
Typically, with the Flying Eye Hospital, we would go to a capital city, or to one city. But with this, we were able to open it up to a much wider audience
I expected the access to the courses to be more challenging. We have some places where connectivity wasn't great. But actually, the participants were so engaged that after their shift they would get together with colleagues they had been working with on that shift, and watch using the hospital's WIFI. And so, we were able to shift the times of the live sessions to accommodate that. It actually turned into an opportunity.
Typically, with the Flying Eye Hospital, we would go to a capital city, or to one city. But with this, we were able to open it up to a much wider audience. We did a course in biomedical engineering, which initially was for the engineers of our partners in Zambia. But because this was remote training, we were able to open that up to partners from right across Africa.
6. Something that we've been working towards, and that has probably accelerated this year, is this idea of combining remote online learning with the in-person, hands-on, surgical skills transfer.
We're very much looking at a blended approach, where we take the best of both, and combine those into one comprehensive training plan. So, our training projects in the future won't just be the three or four weeks that we can physically be in a country. It'll be remote training leading up to that, and potentially remote training afterwards as well. I think there are great lessons learned, and opportunities to take from this experience.
- As told to Lucy Miller.

Comments (0)
You must be logged in to join the discussion. Log in