- OT
- CPD and education
- Capturing the image
Capturing the image
Dr Neelam Patel provides an insight in to how to capture the perfect OCT scan image

07 March 2019
Before getting down to the business of taking the scan, begin by introducing yourself and briefly explain to the patient that you will be taking an OCT scan of their retina.
Patients that are new to this can be reassured that the process involves simply looking at a target and that the scan doesn’t hurt or touch the eye. To capture suitable images the patient must be positioned correctly at a comfortable height, with their chin and forehead on the appropriate support rests. Explain that they will need to stay in this position for a few minutes, so it is important to get their posture right at this stage.
Candle lit dinner for two
Dimming the room lights will help to enlarge the pupil. Some of the newer OCT instruments will automatically align themselves to the patient’s pupil and focus on the retina, otherwise you’ll need to familiarise yourself with the controls to do this manually. The patient will have a fixation target to look at to help keep their line of sight in the correct position. The fixation target may change in appearance and position depending on the type of scan you are taking. It is useful to describe the fixation target and ask the patient to keep looking towards it. At this stage the patient can blink as normal. If they cannot see the fixation target due to poor sight or an eye turn then you’ll need to use the external fixation target. The external fixation target works by providing the other eye with a target to look at and can be moved into different positions until you have the desired alignment for the ‘testing’ eye.
Figure 1a
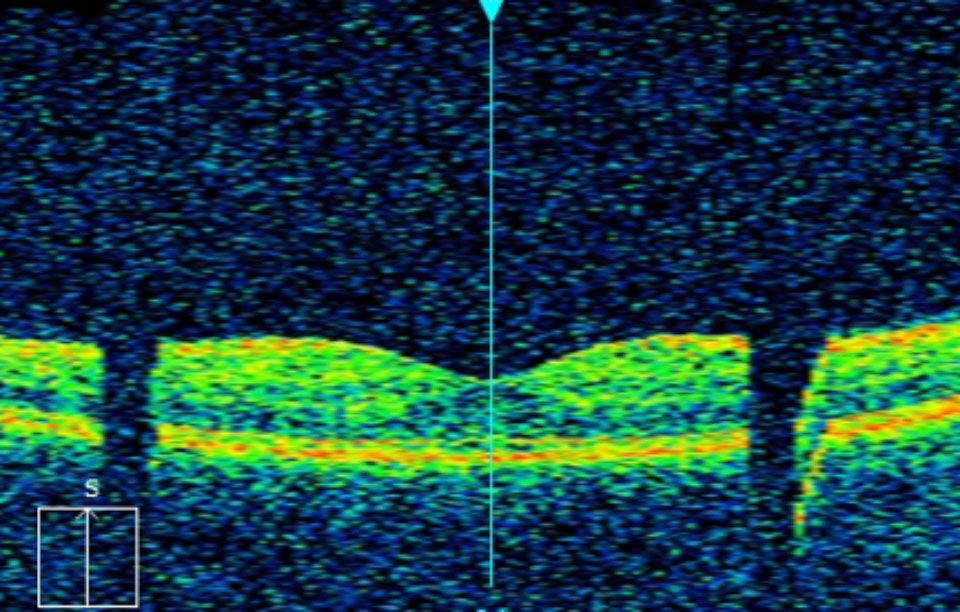
Many OCTs will have a screen that displays a ‘live feed’ of the image. There are usually settings to enhance the image before capturing. Media opacities such as cataract and vitreous floaters may limit how well you can optimise the image. If the pupils are large enough, you could try to move the alignment to another area of the pupil to avoid the media opacities. If this does not help, the patient may require pupil dilation to achieve a more acceptable OCT scan.
Figure 1b
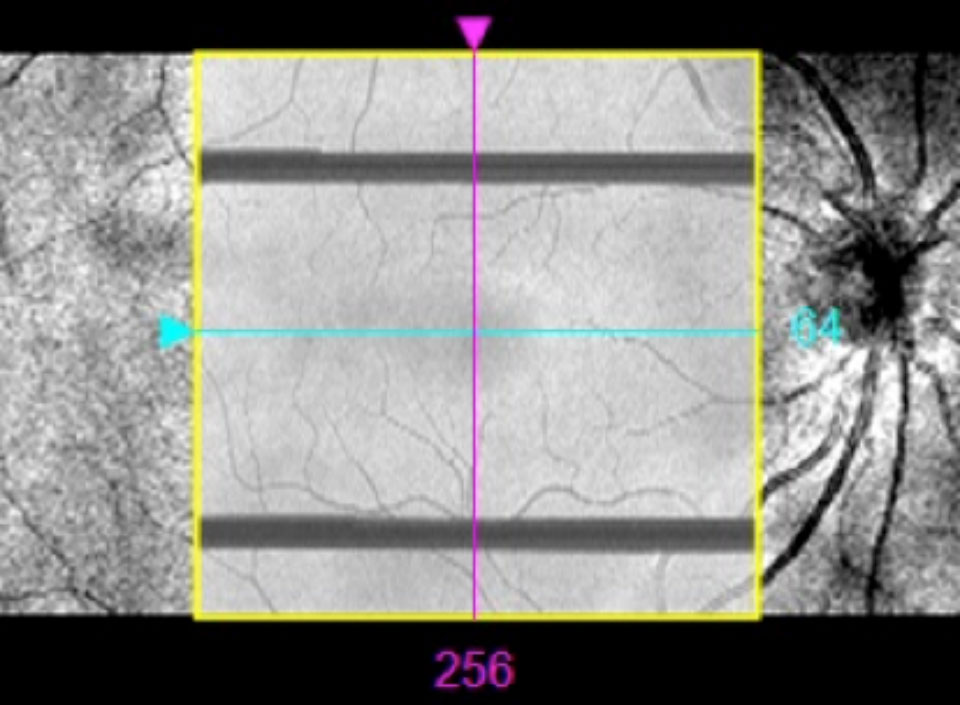
Ready, aim, fire
Capturing the image takes just a few moments. In this time the patient should be instructed to not blink and to keep both eyes wide open. Although you are imaging one eye at a time, keeping both eyes wide open will help reduce blinks and lid closure. Patients with dry eye can use ocular lubricant eye drops to minimise any excessive blinking. The patient should keep looking at the fixation target and try not to move their eyes or become distracted. Once the capture is complete, they can blink as normal again, but advise the patient to stay in the same position as you may need to re-take the image or take additional scans.
Figure 2
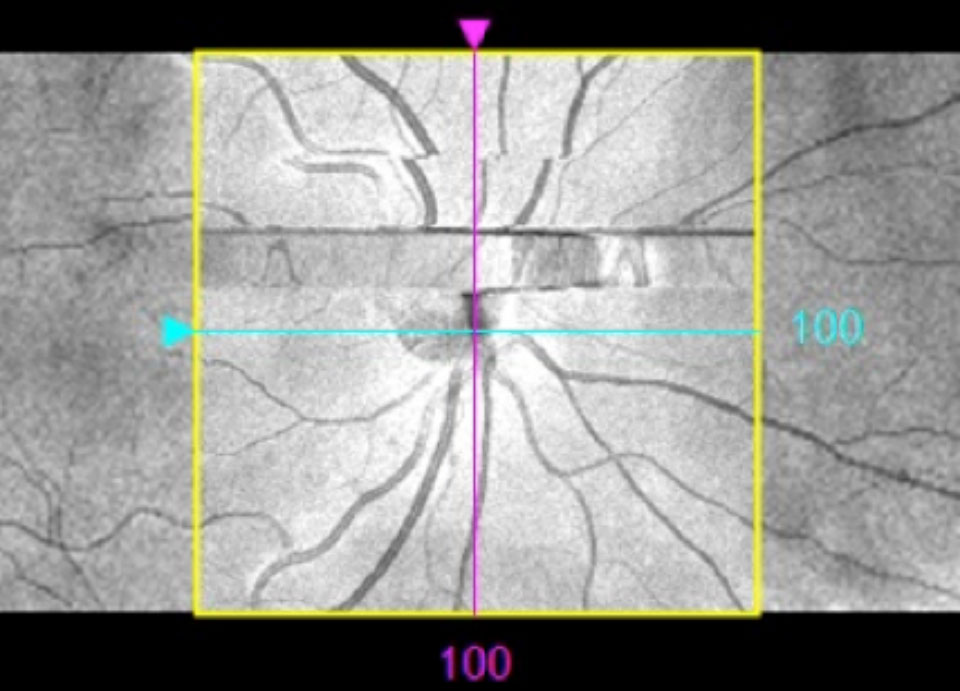
Quality check
After the OCT image has been captured it will usually be displayed on the monitor. It is important to assess the image to ensure that it is of suitable quality with no artefacts. Many OCTs will show a signal-strength score for each scan and this is an indicator of image quality. If the signal strength is high the image will appear distinct and clear. An image with low signal strength will seem grainy and faint. The manufacturer will be able to advise on what signal strength score you should aim for. Common artefacts to look out for include those associated with blinks, motion and incomplete scans. A blink artefact will cause loss of data and so part of the scan will be missing. Blink artefacts are seen as black horizontal bands on the en face image (see Figure 1b) or lost data when scrolling through the B-scan (see Figure 1a). A motion artefact will cause the B-scan to ‘jump’ position when scrolling through and will appear as misalignments of the blood vessels on the en face image (see Figure 2). Incomplete scans may have peripheral areas missing from the en face image or the top or bottom section missing from the B-scan. Incomplete scans can be avoided by repositioning and refocusing. Avoiding artefacts is important as it can render misleading results and may affect clinical decisions and patient management plans. Any significant artefact requires a repeated scan.
Other articles in this series
- 'Selling' the OCT concept to patients: Dr Neelam Patel's three points that every practice team should consider
- The OA's take: Zoe Harrison's views on developing your clinical skillset
- The ABC of OCT: Dr Louise Terry's back-to-basics guide to OCT
- Fact from fiction: From visual fields to AMD, OT gets myth-busting
- The shape of things to come: OCT is evolving and OT explores the trends
- Patient outcomes: Dr Louise Terry on how OCT devices are helping to detect eye conditions
- My take on...OCT: Our experts' predictions on what is next for OCT.
Image credit: Heidelberg Engineering



Comments (0)
You must be logged in to join the discussion. Log in