- OT
- Life in practice
- Practitioner stories
- Experiencing eye care in India
Experiencing eye care in India
Optometry student at City, University of London, Saira Saleem, shares her experience of a two-week work placement at an eye clinic in India

Saira Saleem
17 April 2020
After an intense selection process of applications and an interview, I was thrilled to hear that I had been selected, alongside three other optometry students, to take part in a two-week placement at the LV Prasad Eye Institute (LVPEI) in Hyderabad, India.
It had been seven years since my last visit to India and being from an Indian background myself, I was particularly excited to get in touch with my roots and experience the culture, whilst expanding my educational horizons at the eye hospital.
Previous work experience at various High Street practices has given me insight into the pivotal role of an optometrist in diagnosing and treating various eye conditions such as age-related macular degeneration, cataracts and glaucoma. Knowing these are common conditions that are encountered regularly on a daily basis, I was incredibly excited to see first-hand the more complex ocular conditions that can affect people.

The two-week placement at LVPEI provided me with an opportunity to learn abroad in a completely new environment with people from different parts of the world.
With a lack of easy access to treatment and surgery facilities for conditions such as cataracts, it came as no surprise to me that cataracts are responsible for over 60% of visual impairment in India.
In the UK, conditions such as age-related macular degeneration, which are potentially sight threatening, can be detected early with regular check-ups. However, in India, many cases are left untreated to the point of no return, especially in more rural areas.
In the past I have witnessed first-hand the effects of not having immediate access to eye care when my grandfather was diagnosed with glaucoma. Living in a rural area in India, there weren’t the facilities to appropriately diagnose and treat his glaucoma symptoms. He was required to travel to the LVPEI for an expert opinion, which prolonged the efficient treatment of his condition.
With this in mind, I was eager to witness LVPEI in action with its ongoing projects such as the Vision 2020 initiative that pledges to eliminate avoidable visual impairment to a level that it ceases to be a public health problem.
I was horrified that one patient had thought it was sensible to clean her soft monthly contact lenses with Dettol and go on to repeatedly sleep in them. It came as no surprise that she was experiencing redness and irritation when wearing the contact lenses
Challenges
I saw the placement at LVPEI as an opportunity to develop my knowledge in a world class Institute. Despite my anticipation, travelling abroad to live in a foreign country to gain experience in a fast-paced, pressure-packed environment is something I had never done before.
As my nerves dissolved, the unfamiliarity gave way to friendship. Some of the challenges we faced while in India included adapting to a new system – hospital interns were up and ready for lectures at 7am and continued to work in the clinics until 7pm.
It was eye opening to see just how hard working all the interns were and how meticulous they were with their sound knowledge of all things ‘eyes.’

Learning at LVPEI
During our time at the hospital, we carried out clinical observations in a range of eye health areas: from paediatrics to contact lenses and glaucoma to live eye surgery We were even able to assist examining and testing the patients.
I also observed how the different eye health professionals worked together to deal with a problem, observing how they interacted with patients and one another.
It was interesting to see how the eye examinations in India differed from that in the UK. For example, tumbling Es were used quite commonly for those who were unable to read English. In the UK, we use the duochrome, while in India they tended to get the patient to focus on the 6/60 letter. Cross cylinder work seemed to be unheard of at the Institute, with fan and block the preferred method. Instead of a non-contact tonometer, they opted for either i-care or Goldmann.
It was also interesting to see the stereopsis tests that we learnt about in our binocular vision lectures at university being used in the squint and strabismus clinic. This was previously something I thought wasn’t used often in practice and might not be important, but during the placement I saw how the Randot stereo test was used to diagnose suppression in a child with manifest strabismus.
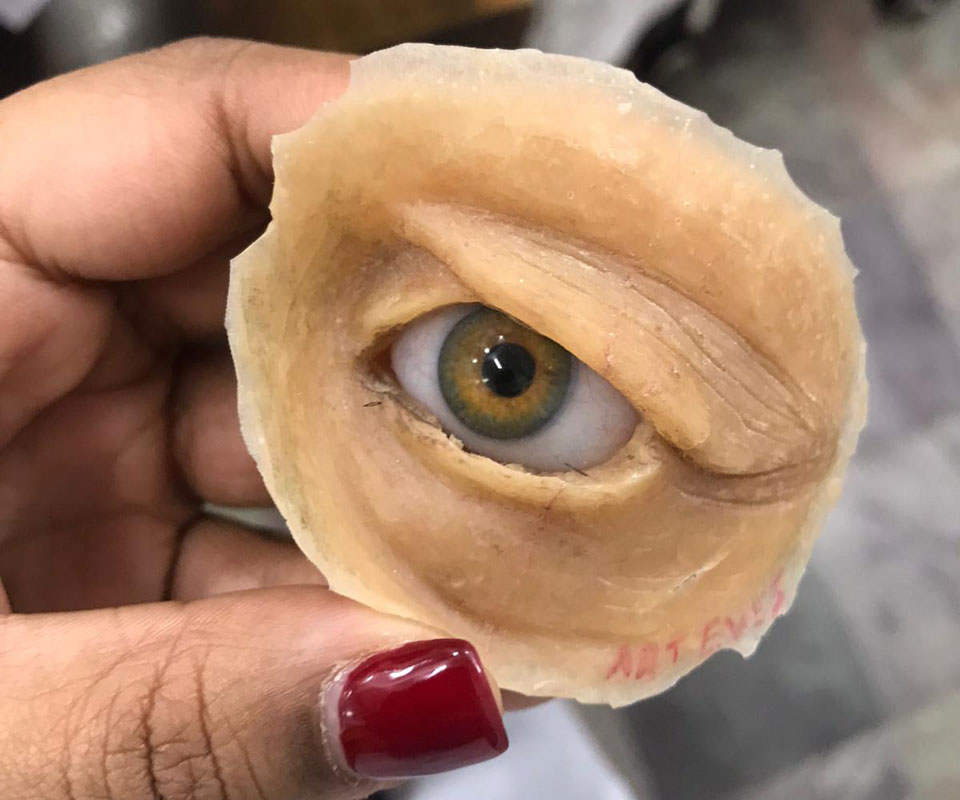
As India is a developing country, we were able to witness rare eye-related cases and oversee their management, something which we would never dream of seeing day-to-day in the UK.
One interesting case we came across was a man had been attacked with an iron rod, leaving his eye damaged beyond repair. His cornea had torn completely and all that could be seen was the white of his sclera. He needed a prosthetic eye and we got to see the process of how the prosthetic eye is made and fitted.
I expected a standard day in the contact lens clinic, but was able to see my first rigid gas permeable and scleral lens fitting. I was horrified that one patient had thought it was sensible to clean her soft monthly contact lenses with Dettol and go on to repeatedly sleep in them. It came as no surprise that she was experiencing redness and irritation when wearing the contact lenses.
In the low vision clinic, I saw a patient who as a result of his anti-TB treatment developed ethambutol toxicity, leading to optic neuritis and greatly reduced vision. The optometrist tried various magnifiers, such as a digital video magnifier and a dome magnifier, in an effort to assist his reading. A number of colour filters were also tried. The patient left relieved that he would be able to continue reading his newspaper every morning with the help of the digital video magnifier.
Witnessing cataract and glaucoma surgery being performed was a truly profound experience. Aside from watching in awe as the surgeons so steadily and efficiently made their incisions, it was fairly amusing to see the painstaking surgeries happening in flipflops in an attempt to keep the wards sterilised.
Working at the LVPEI did not fail to meet my expectations. It allowed me to expand on my depth of knowledge and develop a deeper understanding of the rarer conditions that can be encountered in optometric practice
On my final day in the cornea clinic I saw someone who had recently had a corneal graft, which unfortunately had rejected. However, practitioners were amazed to see how well the patient had recovered after the initial corneal graft rejection. On closer inspection with a slit lamp, I saw the patient had a conjunctival xerosis, which I remembered from a lecture develops from a vitamin A deficiency.
Working at the LVPEI did not fail to meet my expectations. It allowed me to expand on my depth of knowledge and develop a deeper understanding of the rarer conditions that can be encountered in optometric practice. This, as well as interacting with clinical optometry experts overseas, will hopefully assist in moulding me into a well-rounded and competent practitioner in the future.
I’m grateful to City, University of London, the Saturday Hospital Fund and LVPEI, without whom this experience wouldn’t have been possible.
Advertisement

Comments (0)
You must be logged in to join the discussion. Log in