- OT
- Industry
- Equipment and suppliers
- Identifying glaucoma
Advertorial
Identifying glaucoma
Heidelberg Engineering discusses using asymmetry to identify glaucoma
Advertorial content is paid for and produced by a sponsor, and is reviewed and edited by the OT team before publication.
21 June 2017
Macular thickness measurements can be used to identify glaucomatous optic neuropathy due to the loss of the retinal nerve fibre layer (RNFL), ganglion cell bodies and the inner plexiform layer (IPL), which causes thinning of the retina. Total retinal thickness can be assessed relatively easily and accurately using Optical Coherence Tomography (OCT), while some devices, such as the Spectralis, even permit measurement of the thickness of the individual retinal layers.
Glaucoma is typically a bilateral disease, but is frequently asymmetric. A hallmark of glaucoma is asymmetric retinal thinning between the superior and inferior hemispheres of the eye and also asymmetric retinal thinning between the two eyes.
OCT macular thickness maps can be used to compare asymmetry between the superior and inferior macular and also asymmetry between the two eyes to aid in the identification of glaucoma. Pattern recognition of the characteristic arcuate losses on macular thickness maps permits early detection of disease (see Figure 1). It can also help the optometrist to differentiate between glaucoma and other optic neuropathies. For example, the pattern and rate of thinning seen in an MS patient is marked different from a glaucoma patient.
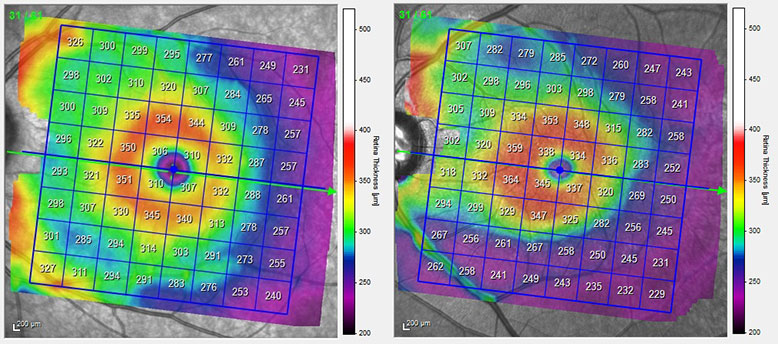
Figure 1: A posterior pole map showing retinal thickness in a normal eye (left) and an eye with glaucoma (right) taken using the Spectralis.
There are limitations to asymmetry analysis. For example, if a co-existing pathology occurs, such as epiretinal membrane, the segmentation of the retinal layers may not be accurate. This could cause the appearance of artificial retinal thickening or thinning. The segmentation of the retinal layers should therefore always be checked carefully when using retinal thickness maps.
You can watch a video on using OCT to assess a patient for glaucoma below.


