- OT
- Industry
- Contact lenses
- The ins and outs of orthokeratology
Advertorial
The ins and outs of orthokeratology
Pauline Bradford discusses the benefits of introducing orthokeratology in practice


Advertorial content is paid for and produced by a sponsor, and is reviewed and edited by the OT team before publication.
03 July 2018
Orthokeratology has been one of the biggest innovations in the contact lens market during the last decade. But what is all the fuss about?
Firstly, it is a non-surgical procedure, which offers the advantage of reduced risk compared to refractive surgery. To the patient, it provides the benefit of being able to see clearly whilst wearing no ocular correction during the day, which has been shown to enhance quality of life. It can be particularly beneficial to those who have experienced discomfort during daily wear of contact lenses, or who take part in sports.1,2
How does it work?
The patient wears an orthokeratology lens overnight (see Figure 1), and corneal epithelial tissue is redistributed using a combination of push and pull forces. This temporarily alters the corneal geometry, and therefore its refracting power. The lens is removed in the morning and the effects should last all day.
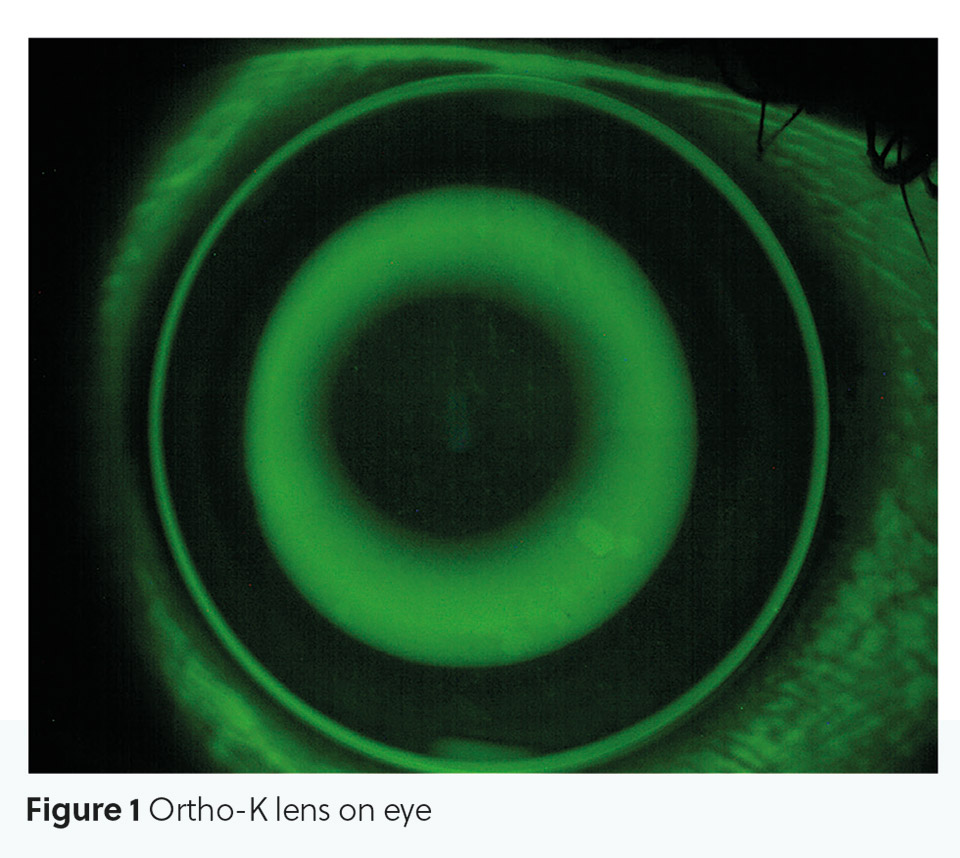
Is any special equipment needed to fit these lenses?
A corneal topographer is needed to fit orthokeratology because K readings only measure a small area of the central cornea. We need more information about the geometry of the peripheral cornea to ensure a good fit, which is required for a good visual outcome. Topography is also used for ongoing monitoring of the corneal shape (see Figure 2).
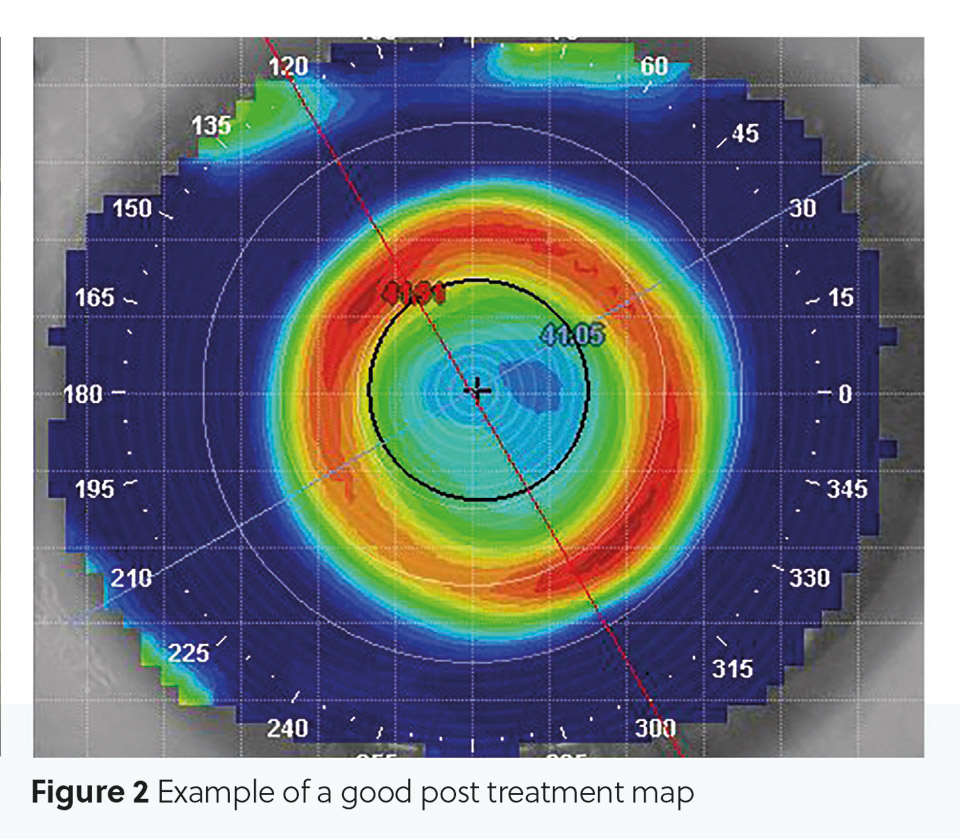
What about myopia management?
Children obtain the same benefits from orthokeratology as adults – clear vision without spectacles or lenses during the day. There is also the added advantage over daily wear lenses that all handling takes place at home, allowing the parent more control over the process. Some eye care practitioners may also choose to fit orthokeratology for children as it has been demonstrated many times to help to control the progression of myopia, reducing the risks of myopia related complications later on in life.3
Who is suitable?
Most orthokeratology lenses are suitable for myopes between -1.00 and -4.00 and cyls to 1.50 (with the rule) and 0.75 (against the rule). Some of the newer designs that have reached market can correct higher levels of myopia, potentially up to -10.00, and cyls to 2.50. However, these higher prescriptions require more skill to achieve a good result and therefore tend to be undertaken by a more experienced eye care practitioner.
About the author
Pauline Bradford has been a contact lens optician since 1994, and has extensive experience of contact lens practice, including specialist and complex fitting. She has been delivering contact lens education since 2013 and now divides her time between contact lens practice and working as a professional services consultant for Bausch + Lomb. She is also a probationary contact lens practical examiner for ABDO.
References
- Lipson, M. J. (2017) Contact Lens Spectrum: Orthokeratology Today, Eyes too dry for contact lenses? Prescribe Ortho–K. Accessed 16 May 2018
- Lipson, M., Sugar, A. and Musch, D. (2005). Overnight Corneal Reshaping Versus Soft Disposable Contact Lenses: Vision-Related Quality-Of-Life Differences from a Randomized Clinical Trial. Optometry and Vision Science, 82(10), Pp.886-891
- Gifford, P. and Gifford, K. (2016). The Future of Myopia Control Contact Lenses. Optometry and Vision Science, 93(4), pp.336-343.


