- OT
- Life in practice
- Practitioner stories
- “It has given us a lot more respect for life”
An optometrist saved my life
“It has given us a lot more respect for life”
Optometrist and director at Specsavers Opticians Leigh, Rumit Patel, and Kelly Morris, mum to eight-year-old Hollie Creighton (pictured), discuss how an emergency appointment for a suspected lazy eye led to the detection of end-stage papilloedema

07 September 2020
Before you went for a sight test, had Hollie experienced any symptoms and how had this affected her in day-to-day life?
Kelly Morris (KM): It started off with headaches. Lockdown kicked in so we didn’t go out and as the weeks went on she became more withdrawn. She was quite happy to stay in bed and watch television, or sleep in a lot more and wasn’t that bothered about getting dressed. When we were allowed to go for walks, it was hard to motivate her to as she just wanted to stay in bed.
I had put it down to the fact that perhaps lockdown had emphasised her anxiety and she also suffers with hayfever and has had headaches with it in the past, so I thought it was that.
One morning she woke up and was sick about two or three times, but then she was fine. Then two weeks later, she was sick again in the morning, but I had seen a post on social media to say there was a sick bug going around, so I assumed it was that.
Then, when we were able to meet up with family in the garden, we took a walk to my mum’s house and she noticed that Hollie’s left eye kept flitting in and going back out again, which I hadn’t noticed. From there it progressed. She kept feeling dizzy, her balance wasn’t right and her eye went really bad. That’s what made me want to get it checked, because I thought it was a lazy eye.
How did COVID-19 affect the way you accessed the services you needed from your optometrist?
KM: I made the appointment online. The lady rang me to say I had made an appointment but my daughter wasn't due an eye test and they were only doing emergency appointments, so I explained the situation. She said they would get her checked and moved the appointment a few days earlier.
It was the first time we had ventured that far - we'd not been into supermarkets as our shopping had been delivered. The doors were closed, the gentleman came to the door; we had to do the two-metre distancing, sanitise our hands and put on masks.
It made us feel at ease. We didn't feel strange, we felt welcomed and they checked we were okay.
It was breaking my heart, because I was expecting a lazy eye – not that there was something wrong with her brain
What did the optometrist find, and how did they explain the next steps to you?
KM: Rumit brought us in to check her eyes and found her eyesight was fine, but he could obviously see there was something not right with her left eye.
He left the room for about five minutes, explaining that he just needed to have a look at the pictures of the back of her eye again. When he came back he asked if he could speak to me on my own. I knew then there was something.
We sat Hollie in the waiting room with cartoons on and he explained it to me, with the pictures showing the back of her eye. When she’d been in for a sight test in November, she had the white disc there – and now it had completely disappeared. This suggested there was pressure on the brain and something was causing that pressure.
He explained that he wanted to email the pictures to a consultant at Leigh Infirmary, who would get in touch and would be able to find out the cause of the pressure.
It was breaking my heart, because I was expecting a lazy eye – not that there was something wrong with her brain.
Rumit was lovely and told us to go home and make sure the phone was on. He said: “I’m sorry I’ve had to give you this bad news, but I’m really glad you’ve come in today.”
I told him, “So am I.”
Can you describe how you felt during the referral?
KM: I got the phone call at about 3pm from Leigh Infirmary. The consultant had seen the email and images of Hollie's eyes and suggested we take her to the paediatrics department at Wigan Hospital right away. They said they would ring ahead to let them know we are on the way. I knew then that it was serious.
At the hospital we had a CET scan done and the doctor asked to speak to me on my own. My heart sank, and I thought, can it get any worse?
They explained there was a tumour at the back of Hollie’s spine where the cerebral nerves are. They had sent the pictures over to a consultant at Manchester Children’s Hospital and they wanted us to go there right away to operate as soon as possible.
I asked the doctor to explain it to Hollie and he simplified it by saying that she had a lump at the back of her head and that is what was making her poorly, so we were going to Manchester Hospital where they were going to take it out.
Did Hollie have to undergo treatment and what has been the outcome? Will she need further treatment?
KM: At Manchester Hospital, the surgeon who was doing the operation took us into a room and showed us the scan of where the tumour was. They explained what effect it was having and the urgency of having to get that out, because the pressure was to the point where it wouldn’t be able to go any further. That pressure would have caused irreversible damage.
They came to get her from the ward the next morning and the surgery took six hours.
Since then, she has gone from strength to strength. She’s TikTok-ing, dancing, happy to go for walks most nights now. She’s like a completely different child. It’s great to have her back.
There’s still some swelling, which they are saying they would expect. But the rest of the eye looks good and they are happy with the progress.
I couldn’t praise Rumit enough. He didn’t just do the test, give us the news and send us on our way. He has been in touch the whole way through, checking in on her progress. I suppose you could say it is his job, but it’s not his job to check she’s okay. It just goes to show how much he cares.

How has this experience affected your views on importance of sight tests?
KM: It’s very important. To the point where I realised it had been two years since I had my eyes checked, and I have decided to make an appointment. Even somebody I work with, this has made them think that they need to go and get theirs checked.
Even if you think you have got perfect vision, a sight test isn’t just about whether you can see or not. You can also see the health of your eyes. And like with Hollie’s, it can pick up things you wouldn’t think it could.
For something like a simple headache, it’s not always going to be something serious – but you just never know and there is no harm in checking. There is more harm in not checking.
How has this experience impacted your lives?
KM: It has given us a lot more respect for life. It does go to show how fragile life is, and not to waste it.
I am always one for making memories and making the most of precious people and moments. It’s been hard with lockdown, but it doesn’t stop you from cherishing those that are in your life.
It definitely gives you a different outlook on life.
She has gone from strength to strength. She’s TikTok-ing, dancing, happy to go for walks most nights now. She’s like a completely different child. It’s great to have her back
How has COVID-19 affected your practice, and how did you adjust your services/approach to be able to meet the needs of your patients, such as in this case?
Rumit Patel (RP): COVID-19 has hugely affected our practice and how we operate. The first few months were difficult as it was just myself, my business partner, Mathew and store manager, Alex attending to our patients’ clinical needs. All other staff members were put on the furlough scheme.
We have been open for urgent, emergency care and now, as restrictions lifted, essential and routine. We wanted to reduce the strain on the GP practices, walk-in centres and NHS hospitals by attending to our patients via telephone triaging or face-to-face consultation if deemed necessary.
We put in place, and still adhere to, social distancing guidelines by removing dispensing tables and chairs, rearranging waiting area space and adopting a meet and greeter at the front of practice.
When young Hollie attended the practice on the Thursday 4 June, we were still unable to see routine eye examinations but were able to see Hollie as her symptoms were of an urgent and emergency nature.
At the time I was running a single clinic and managing it myself, welcoming, pre-screening and testing my own patients.
When Hollie attended for her examination, I was slightly surprised, as we were not seeing many appointments with children at the time. Kelly, her mother, booked her in because she was having acute symptoms of headaches, pain, blurry vision, and she had noticed that over four weeks, Hollie’s left eye had drifted inwards.
I was in deep shock and quite emotional because, having been qualified for over 15 years, it was so unexpected
What did you identify during the sight test and what was your reaction?
RP: When Hollie attended her appointment, she was clearly in distress and discomfort. She suffers with separation anxiety and therefore needed her mum to be with her whilst I took her fundus images and conducted the pre-test.
I asked Hollie why she was so upset, and her response was, “It hurts, it really hurts, my eye” pointing to her left eye, which was the one Kelly had noticed had drifted inwards.
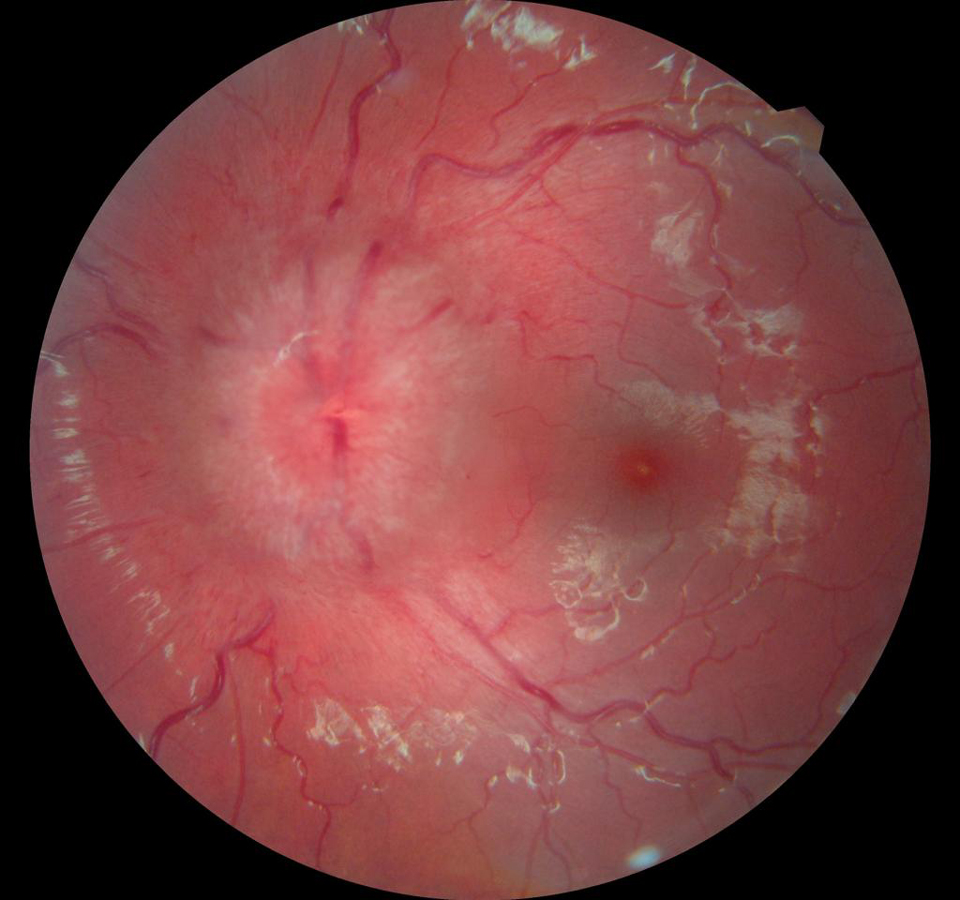
I had seen the fundus images of Hollie’s retina prior to taking her through for the examination and compared them to her previous visit in November 2019, where her optic disc margins were clearly distinct.
I identified she had end-stage papilloedema, based on her fundus images, the fact her left eye drifted inwards, poor pupil responses and her symptoms.
I was in deep shock and quite emotional because, having been qualified for over 15 years, it was so unexpected. I really felt for her and her mum.
How do you approach explaining what you had identified?
RP: Before explaining to Kelly that I had to refer Hollie urgently, I stepped out to get some fresh air for a minute or two in order to compose myself and to find the correct words to tell Kelly without making her panic or putting her in any distress.
I asked Hollie if she wouldn't mind watching television in the waiting area whilst I had a conversation with Kelly. When I did, I was composed and consciously did not use the wording or language of anything that could signify a potential tumour.
I explained the fundus photo images and described the features to her. I did specify that the reason the optic disc margins looked different to when she attended her last eye test was due to a build of pressure underneath the optic disc, but I didn't go into the specifics of what that could be caused by.
I advised her I would refer her urgently to someone to investigate her symptoms in more detail and for extra tests to be conducted to find the cause of her discomfort.
What were the next steps that you took, and what was the significance of these steps to this case?
RP: In our area, when we see any urgent eye cases, the protocol is to refer the patient urgently, via email, to Leigh and Wigan Infirmary through to a triage centre at the hospital.
They triage the referrals and contact the patient directly to arrange an appointment to see the ophthalmologist as soon as is deemed necessary.
In this case, I attached her fundus images to her referral letter and emailed it across immediately.
I then followed it up later in the day and had a reply from the clinic co-ordinator, Kay Conway, who advised me that the consultant had triaged my referral and advised Hollie to attend paediatrics A+E immediately.
Kelly and Hollie have popped into the store to see me on a few occasions since, which has been amazing, and she is recovering tremendously well. She’s a different child to the one who came into see me in June
When did you hear about the results of your referral and how have you been involved since?
RP: I was in constant contact with Kelly throughout the 24 hours and she was keeping me updated via text or phone calls.
Since referring Hollie, I am still in regular contact with Kelly to see how her recovery is going and how her health is.
Kelly and Hollie have popped into the store to see me on a few occasions since, which has been amazing, and she is recovering tremendously well. She’s a different child to the one who came into see me in June.
What would be your three top tips to other practitioners when making a referral, either generally or during COVID-19?
RP: 1. Be clear and transparent with your referral letter, to either a triage centre or a consultant directly, and put in as much information as you can
2. If you’re not sure what the diagnosis is, then don’t diagnose, describe what you see or what you hear
3. Don’t be shy or scared to ask for help. If you’re unsure or in doubt, ask.
You have been sharing this experience alongside Kelly with the aim of raising awareness with families. What would be your key message?
RP: My message is a simple one: listen, hear and do not ignore your child’s symptoms. Other parents may have ignored these symptoms, or visited the GP when it was too late.
If your child is in distress, seek medical care immediately. This is not specific to myself as an optometrist, it also applies to medical practitioners, pharmacists, dentist – all health care workers. We are all here to help.
If your child has a headache, do not dismiss it or be too quick to blame it on excessive phone or tablet-use or gaming. Do take it seriously and please seek assistance or help if needed.
The experience Hollie and Kelly have been through has been life changing, and I hope that by sharing their experience, it will help the next parent or child think differently.
Advertisement


Comments (0)
You must be logged in to join the discussion. Log in