- OT
- Life in practice
- Career development
- The locum optometrist’s toolkit
Locum optometrist guide
The locum optometrist’s toolkit
From contract negotiation to further qualifications, OT identifies the skills to help locums adapt and thrive amid a shifting professional landscape

16 December 2020
Adaptability is a quality that stands a locum optometrist in good stead.
In a job where a locum might work in a different practice each day of the week, locum optometrists need to be able to shift seamlessly between different technology, processes and team dynamics.
In the broader context of the pandemic, the ability to be flexible has never been more important for locums. Social distancing has restricted the number of patients who can be seen in practice and increased the competition for available work.
So how can locums best hone and market their skillset? OT canvasses industry experts and locums from across the UK for their tips.
Meet the panel
Location: Leicester
Years qualified: Three
Name: Prinal Patel
Location: West Sussex/Surrey
Years qualified: 11
Name: Craig McCoy
Location: Aberdeen
Years qualified: Six
Name: Kris Cottier
Location: Kent
Years qualified: 21
Name: Rebecca Rushton
Location: Southampton
Years qualified: 15
Name: Andrea Mentlikowski
Location: London
Years qualified: 22
1. Finding and keeping work
When it comes to securing work, AOP Awards locum of the year, Prinal Patel, recommends working with a variety of agencies, speaking with colleagues and checking the websites of professional bodies, such as the AOP, for locum advertisements.
While Ms Patel has worked less during the pandemic, she has not had to reduce her rates.
Aberdeen-based locum, Craig McCoy, shared that when he started as a locum, he sent letters to independent practices in the region where he was working.
He highlighted that word of mouth has been his most effective way of finding work, although he has also created a website and is listed on the AOP locum register.

“I’ve had time to re-think my strategy,” she shared.
“To find a good job, strive to be the best and let employers know you’re the best. Upskill and consider specialising,” Ms Rushton said.
Putting work into her LinkedIn profile has helped Ms Rushton to secure work.
Once a locum first works for a practice, how can they ensure that the practice manager is keen to call them back if further work becomes available?
Ms Rushton highlighted the need to provide the best possible customer service, patient care and value to the business.
“Be kind and friendly with the staff, offering to help them where you can. Flexibility is key, now more so than ever,” she said.

“As soon as you step foot in the door, be conscious that you’re part of that team,” he said.
“I make every effort to try to get to know the staff and introduce myself to each member. I often find that works well and eases you into the day,” Mr Safdar highlighted.
He discouraged colleagues from falling back on the excuse that they are ‘just a locum.’
“You’re an eye health professional just like the peers you’re covering for, and should be treated the same,” Mr Safdar said.
AOP support
The AOP has two complementary member resources for locums looking for work within the UK.
The AOP locum vacancies list enables members to advertise and search for locum positions free of charge, while members can list their availability for locum work on the AOP locum register.
Find out more on the website:
www.aop.org.uk/locum-vacancies
www.aop.org.uk/advice-and-support/business/aop-locum-register
2. Negotiating a fair rate
With fewer patients coming through practices, the availability of locum work became more scarce following the outbreak of COVID-19.
Anecdotally, there were reports that locum optometrists were being offered much lower rates than they would usually expect.
So how can locum optometrists ensure that their work is remunerated at an appropriate rate?
AOP clinical director, Dr Peter Hampson, emphasised that the most important point when negotiating pay rates is to know what a practitioner brings to the business, whether that’s clinical skills, dispensing support, the ability to provide short notice cover or great communication skills.
“Don’t be afraid to let people know your strengths,” Dr Hampson said.He highlighted that locums needed to take a realistic attitude to pay rates.
“Depending on where in the country you are located, the rates will vary. Some areas are harder to cover than others and some shifts are less desirable than others. Make sure the rate you are asking is comparable to others in your area,” Dr Hampson advised.
He added that as a self-employed worker, locums can pick and choose what work they take – so if the rate is not acceptable they have the option of declining work.
When negotiating work with a practice, locums should be clear what time they start and finish, and when their breaks will be.
“Preferably set a maximum number of appointments and how long those appointments will be. It also helps to get these terms in writing, for two main reasons: it manages expectations and if someone tries to make you work in a different way you can lean on the written evidence,” Dr Hampson explained.
He added that managers often have not made the locum booking themselves so may not be aware of the details of the booking.
“If you have your terms in writing you can use this to stick to your position and refuse any unreasonable requests,” Dr Hampson highlighted.
Top negotiating tips
AOP clinical director Dr Peter Hampson shares five pointers for contract negotiation
• Know your own worth and what you bring to the business
• Make sure you are clear in advance on what you will and won’t do
• Set a maximum number of appointments and make sure start and end times, breaks and appointment times are clear
• Get any terms in writing, don’t settle for verbal contracts as they are hard to enforce
• Be prepared to say “no.”
Rates of pay: the locum view
“I believe that a 'fair rate' should be based on your expertise, professionalism and ability to deliver excellent patient care. I would recommend making a list of your attributes and experiences that would help your employer select you as their locum. This will also act as your foundation for negotiating a suitable rate. It is important to consider testing times and conditions of your working environment”
Prinal Patel
“I've always made it clear before working at a practice that I charge based on the service I provide, not the number of tests or specs sold”
Craig McCoy
“Be flexible, willing to understand and appreciate others point of view and the reasoning for their suggested rate. We have all had to learn to adapt to the new way of life during this pandemic, so we must be mindful of the difficulties business will have endured throughout. Understand their position and how you can add value to their practice with your skills and qualities. One approach could be that you would be happy to meet somewhere in the middle for the next few weeks but thereafter return to your normal rate”
Hassnain Safdar
“With the whole industry struggling, now is a time for mutual respect between the employer and the locum”
Kris Cottier
“There has been talk in the locum community about some contractors offering reduced rates, which implies that we are somehow performing a reduced service. I'd argue that at the moment, we are in fact providing an enhanced service, with additional training in the science of COVID-19, how it relates to the eyes and contact lens wear, infection control and personal protective equipment use, and keeping updated with the continuously changing advice for our professional practice”
Andrea Mentlikowski
“Negotiation is the hardest part of being a locum. Know the typical rate in your area and consider what extra value you can offer”
Rebecca Rushton
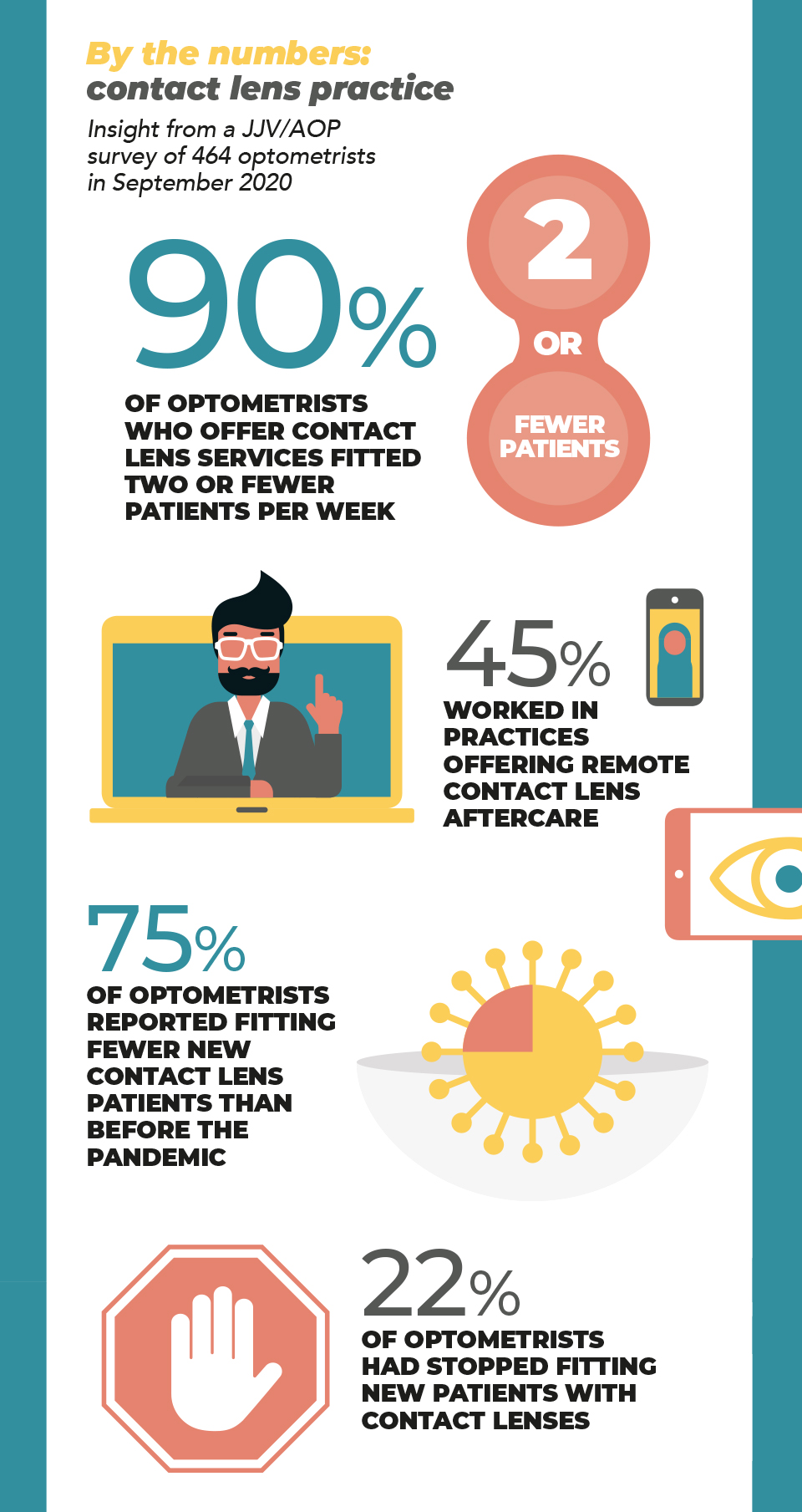
3. Fitting contact lenses during a pandemic
Changes in how people work and socialise following the pandemic have implications for the way that patients use contact lenses.
Professor James Wolffsohn, from Aston University, highlighted that during COVID-19 contact lenses are a practical solution to the problem of spectacle lenses steaming up while wearing a face mask.
He added that the eyes are not a preferred transmission route for COVID-19, while there is no strong evidence that spectacles are more or less safe than contact lens wear when it comes to contracting the virus.
Professor Wolffsohn shared that anterior eye examination – for example, lid eversion – requires optometrists to touch a patient’s skin. This can be done safely using good hygiene procedures.
“The emphasis on good hygiene could be useful for better future patient compliance in this important element of safe contact lens wear,” he said.
Around half of the patients who drop out from contact lens wear will do so in the first couple of months after fitting, Professor Wolffsohn noted.
Digital resources can be used to supplement in-person assistance following a contact lens fit.
“There are good online websites to help teach a patient to apply and remove lenses and a remote consultation can be used to support a patient if necessary,” Professor Wolffsohn shared.
During the pandemic, researchers have described ocular surface problems associated with face mask use.
Professor Wolffsohn noted that Mask Associated Dry Eye is linked to a flow of air being directed over the ocular surface by the mask increasing evaporation and therefore disrupting the homeostasis of the tear film.
“This could be exacerbated in contact lens wearers, especially those wearing lenses with a high water content,” he added.
“A well-fitting mask around the nose, application of ‘surgical’ tape to hold the top of the mask against the skin and the use of artificial tears are remedies that can be discussed with your patients,” Professor Wolffsohn said.
Johnson and Johnson Vision (JJV) professional education and development manager for UK and Ireland, Sheetal Patel, highlighted that contact lens category had remained “relatively resilient” compared to many other sectors.
“There was an initial impact as lockdown was imposed and then there has been an encouraging recovery as practices have reopened. The fact that direct debit subscription is so prevalent has protected sales to a significant degree,” she said.
Cash sales of contact lenses was the area that was most affected, while those who changed subscriptions as a result of COVID-19 generally tended to suspend rather than cancel their subscription.
“It is encouraging to note as it means that patients are still interested in remaining contact lens wearers although perceived demand or occasions for wear may have reduced during the pandemic,” Ms Patel explained.
When asked how lifestyle changes linked to the pandemic have affected contact lens wear, Ms Patel observed that reduced occasions for wearing contact lenses has had an impact on wearer behaviour.
However, there are instances where contact lenses are more favourable than spectacles because of the need to wear masks in certain environments.
She emphasised the importance of eye care professionals talking to patients about the broader benefits of contact lenses in daily activities – not just for big occasions and socialising.
Everyday activities, such as exercise, virtual calls, gardening and hobbies, are often better with contact lenses, Ms Patel observed.
She noted that while there is a backlog of eye examinations as a result of the pandemic, contact lenses are still an important consideration for practices and patients.
“Providing patients with the opportunity for dual wear ensures that not only do they benefit from recommendations based on their unique needs, but businesses also benefit from offering more than one optical solution,” Ms Patel said.
Clarity on contact lenses
Johnson & Johnson Vision’s Sheetal Patel on how eye care professionals can navigate the changes prompted by the pandemic
From an eye care professional perspective there may appear to be confusion around the guidance for contact lens practice and how patients should be fitted, how application and removal should be conducted and, depending on the social distancing measures in place, what is the correct practice to follow.
These factors partly explain why contact lenses are not being fitted as much compared to pre-COVID. In these instances, it would be best to seek clarity from professional bodies like the AOP to ensure that patients’ needs continue to be met and practices also continue to benefit from offering multiple solutions to patients.
Johnson & Johnson Vision also have an informative CET lecture available on their website featuring Professor Phil Morgan discussing contact lens wear and COVID which helps to provide some guidance around contact lens practice and any hygiene concerns at this time.
From a patient perspective the hygiene aspect around contact lens wear and COVID maybe confusing and not well understood. Eye care professionals play a role here to ensure that patients are reassured that contact lens wear is still safe as long as all normal hygiene practices are followed.
Resources
Johnson & Johnson Vision COVID-19 and Contact Lens Wear and Care Webinar
AOP guidance on COVID-19
4. Offering more with qualifications
With more eye conditions being managed in the community to ease the burden on secondary care, many optometrists have embarked on further study to enhance their clinical skillset.
For locums, additional qualifications are part of the value that they bring to a business and may assist in securing work in practices that offer extended eye care services.

She noted that these clinical skills help to build closer working relationships with ophthalmologists and ensure that optometrists are offering the best possible care to patients.
Undertaking further qualifications also helps patients to realise that an optometrist’s role is broader than ‘just glasses,’ Ms Patel added.
“I have a better understanding and ability to engage with patients about their hospital eye care and explain referral processes and treatments,” she said.
Locum Craig McCoy qualified as an independent prescribing (IP) optometrist in 2017 and completed his professional certificate in glaucoma in 2019.
The experience and training he gained through IP has helped to build Mr McCoy’s confidence in managing pathology – which he particularly values as he is often working alone.
“A big part of the course is making management plans that others can follow, though I try never to leave work for someone else to manage if I can avoid it,” he said.
Locum Hassnain Safdar noted that the pandemic has acted as a catalyst for many optometrists to upskill.
“For me, this pandemic has reminded me that the future is highly unpredictable and to make the most of the time at hand,” he shared.
This has led Mr Safdar to pursue an independent prescribing qualification which he has started through the University of Hertfordshire.
Universities offering independent prescribing
City University of London
Cardiff University
Glasgow Caledonian University
University of Hertfordshire
Ulster University

